Some History
I wrote about my first bout with vertigo almost 3 years ago. I had a bad middle ear infection back then which gave me room-spinning dizziness and loss of balance. I was fine for over a year but in June of 2020 I woke up to the same symptoms. I didn't even have an ear infection with this episode. I was taken to my local urgent care and received the same treatment: anti-nausea and anti-dizziness meds. I was sent home and took 2 days to get over it.
I was, however, referred to an otolaryngologist (an ENT - ear, nose, throat doctor) and saw her at the beginning of August. Hearing tests (audiogram) showed I had some conductive hearing loss in my right ear and confirmed the tinnitus that I've had for about a year and a half. The doctor said that now that I was an established patient, that if I experience another vertigo episode, I could call and probably get a same-day appointment which would be helpful in determining what's going on while it's happening.

Latest Episode
In early December of last year, I had another episode of vertigo and dizziness. Same type of thing - couldn't walk without stumbling, stand without falling, sit up in bed without flopping. Even more annoyingly, my neck pain from a couple years ago was making a comeback. The vertigo itself lasted for 3 days again and of course started on a Saturday, but I was able to see my ENT on the following Monday.
Audiogram this time showed that I had perfect hearing again (the right ear hearing loss was gone). Tinnitus of course was still present. She examined my eyes looking for nystagmus (rapid involuntary side-to-side eye movement), checked my eye tracking, and performed the Dix-Hallpike test which looked negative to her meaning I didn't have BPPV (benign paroxysmal positional vertigo). She asked me if I had a history of migraines which I do, and even this time I felt I had a migraine during this episode. With this information, she suspected that I had a vestibular migraine which is a migraine that may or may not include an actual headache but certainly can involve vertigo among its symptoms. Out of the 14% of the population that have migraines, 1% of those people have migraine associated vertigo - and of them more women are affected than men. There is no test for diagnosing vestibular migraine but she referred me to a hearing and balance center to have some tests done to rule out other causes.
Vestibular Testing Part 1
So later that week, I had a VNG (videonystagmography) done. This involved a series of tests wearing special goggles to record my eyes as I track dots and movement while laying in different positions. One of the tests is called a caloric test, where cold & warm air/water is pumped into my ears one at a time to see how my eyes react (checking for nystagmus). Normal results would create the sensation of vertigo as the test stimulates the acoustic nerve.
All of my tests showed normal response except for the caloric test which showed an abnormal response, specifically bilateral vestibular hypofunction. During my caloric test, I did not experience any vertigo or nystagmus. So with that, my ENT ordered an MRI to be done of my brain and ears to rule out other (and more serious causes).
A few days after the VNG, I had a dentist appointment and I experienced another dizziness episode after 20 minutes of laying back in the chair which was tilted downwards. Although it persisted throughout the procedure, I just wanted to get through the visit so I stuck it out. I couldn't walk let alone drive myself home so my wife had to pick me up (and retrieve my car later). The dizziness waned about an hour after I got home but I felt overall off-balance as I did before.
I had the MRI done and those results luckily showed up, as doctors say, unremarkable. Still on the heels of the possible bilateral vestibular hypofunction diagnosis, I was then suggested to start vestibular rehabilitation - a form of physical therapy that focuses on balance and recalibrating my brain to raise my threshold of getting dizzy. My ENT also got me a referral to an otoneurologist at the Ohio State University Wexner Medical Center who specializes in vestibular diseases & conditions.
Vestibular Rehabilitation
I started my physical therapy this past January and continued through to middle of February. This involved exercises with eye movement, balancing (or at least attempting) on a pivoting platform, standing/stepping on a software surface, motion tracking, and walking with hand motion. The therapist said I was making improvement but it was hard for me to see that as I didn't feel like I was. Throughout February I was feeling especially bad as I was nauseous 24/7 while being upright and moving making it worse. Needless to say with 2 weeks of this, I wasn't able to get through a 30 minute session of physical therapy.
Vestibular Testing Part 2
I traveled to the other side of Columbus for this testing, which included the use of a rotary chair as well as the other vestibular tests done before (Head Impulse Test, caloric, etc). It was an interesting experience, being strapped into the chair and spinning so fast but in complete darkness. I was almost feeling a bit sick to my stomach at times but overall not so bad. The caloric test this time was done with water which felt similar to when I had my ears cleared of impacted cerumen (ear wax).
I waited for about a week before contacting them about the results which I received shortly after. The doctor noted that all of my testing was normal, showing no evidence of bilateral vestibular weakness. I suspect the reason that the first caloric test was abnormal was that: a.) it was done using air which is less sensitive than using water and b.) the air didn't quite make direct contact inside my ears as it's been pointed out to me that my ear canals go sharply upwards while normally they would go slightly upwards before turning back toward my inner ear. So this would cause the acoustic nerves to not register much of anything. My total response was still kind of low but high enough to say it's not a bilateral weakness. The original caloric testing should have been redone to confirm the abnormality.
Diagnosis
He did, however, suggest what my ENT had suspected at first, that I am suffering from vestibular migraines which lead to developing PPPD (persistent postural-perceptual dizziness). The migraines are the episodic "attacks" that leave me unable to function for a few days at a time. The PPPD is a chronic condition of ongoing dizziness symptoms and non-spinning vertigo that is initially caused by a vestibular disorder or disturbance such as the vestibular migraines.

Explaining PPPD
What happens here is that during a vestibular crisis, the brain goes into a high-alert mode trying to overcompensate and fix the issues with dizziness & balance. And when a person gets better, the proper thing is for the brain to get out of this crisis-mode but this time it did not for me. My brain is on constant high alert that I might fall or stumble. It says hyper-vigilant with excessive self-monitoring of motion and continues with over reliance on vision for balance when it could just trust the vestibular (inner ear) and proprioception (signals from legs & feet) systems that I'm not in danger. Essentially communication between my vestibular system and brain is not working correctly.
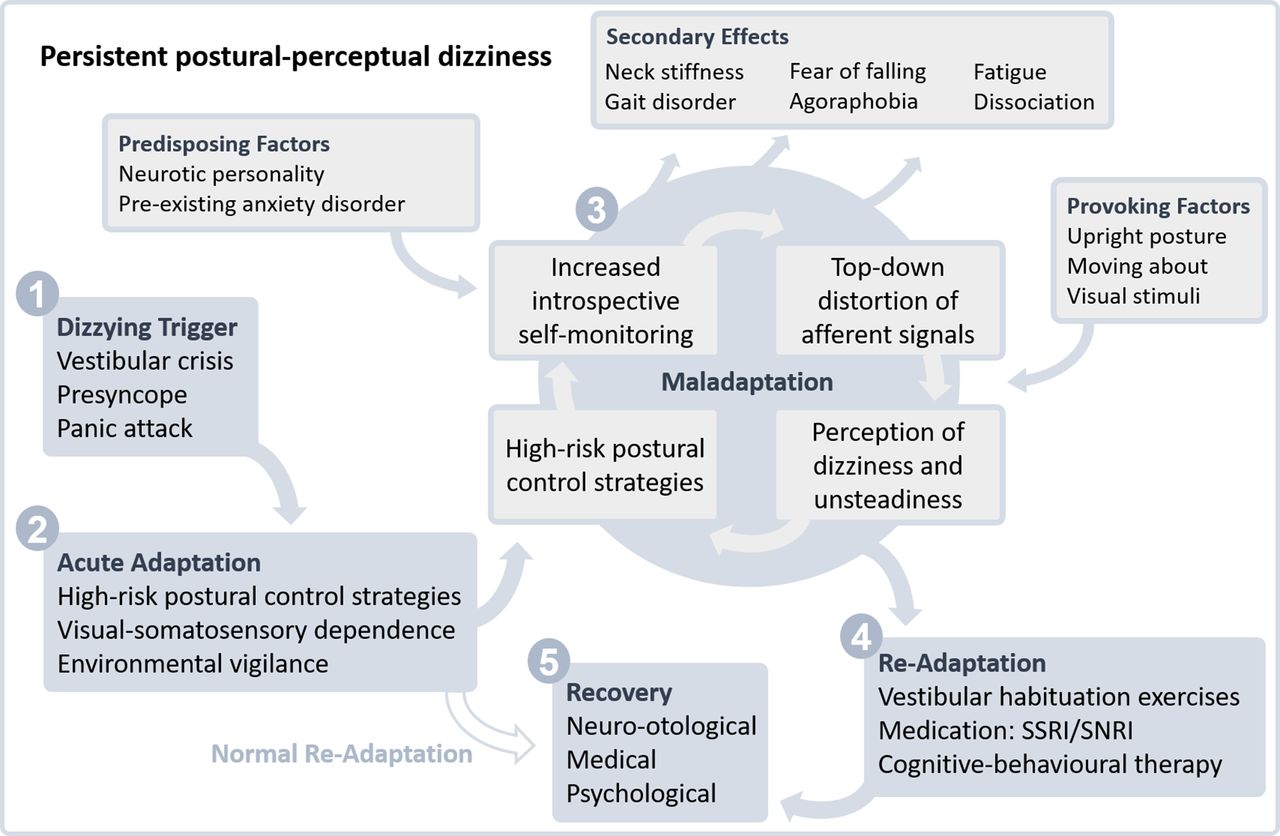
This in turn creates a perpetuating loop of:
- Anxiety of falling/dizziness causing more self-observation like paying more attention to 'keeping balance' and gaze fixation.
- Sensory information about body position is then amplified and distorted by the brain.
- This then produces the dizziness and balance issues one is trying to avoid as well as creating secondary unwanted effects such as muscle tightness in the legs, back, and neck.
- A phobic avoidance of activities can then occur as well as developing mental fatigue.
- Back to #1.
It can sound like this condition is "all in my head" and I should just not worry and just do things normally. But these symptoms are very real and not easy to just "get over":
- non-spinning vertigo (sensation of swaying or rocking even though I'm sitting/standing still)
- unsteadiness (feeling like I'm going to fall and have to catch myself)
- light-headedness
- mild dissociation (feeling 'spaced out' or not connected to the world around me)
- difficulty concentrating / "brain fog"
And all this is excerbated by anxiety and sudden motion (active or passive) and generally worse when I cannot control the motion. Even sitting upright can make me feel worse as well as "busy" environments e.g. crowds, patterned carpets, and contrasting products in store aisles.
And the symptoms can wax and wane, lasting for an extended period of time or not show up again after a few days - this makes it annoyingly unpredictable.
Now combines those with the symptoms of a vestibular migraine episode:
- more balance issues
- motion sensitivity, actively or passively
- spinning and non-spinning vertigo
- sensitivity to visual stimuli
- motion sickness
- near constant nausea

How it's going
So far I have been feeling miserable most of the time with only a few "good days." The brain fog has hit me in the middle of most afternoons and by evening I cannot focus on anything. I feel that the things that I enjoy are being taken away from me or that I cannot do activities as well as I could before all this.
- When I have a vestibular migraine, luckily I haven't had the typical sensitivity to light or sound. However, I am very sensitive to motion where just walking across the room makes me feel dizzy and queasy.
- Work has been slightly more difficult. I finally have a job that I love doing. I'm coding for a living now. However most of programming is thinking, planning, and designing a solution. The concentration/brain fog issue is biting me by mid-afternoon and I'm so angry about it. I want to do my job well but sometimes I just cannot even think.
- Driving is literally nauseating. I cannot drive more than 5 minutes or so without getting motion sickness. I have to avoid making too sharp or fast of a turn or my vision gets a little blurred but it seems to come back as soon as I'm out of the turn. Being a passenger is no picnic either.
- Cooking is slightly more difficult now with how much I need to move from stove, island, and counters - turning around a lot makes me dizzy easily.
- Playing games on the computer or a console is limited to things that isn't fast moving. So at the moment, Mario Kart and close up action is avoided. If I can zoom out to slow it down, I don't feel too bad.
- I cannot quickly scroll through a browser window or my phone. That movement is too fast so I'm going to have to slow down there.
- Reading long passages of text has always been a problem for the past few years (wondering if that's always been a symptom of the migraines) but if it's not short and to the point, I can't focus on it.
- Watching TV or movies longer than a couple of hours triggers bad headaches. With my favorite movies clocking close to 3 hours long, this will get annoying.
- My neck pain is back and I'm wondering if it's because of a pinched nerve like before or the vicious cycle of my PPPD.
- I'm having more occasional migraines, at the least I'm finally recognizing them as migraines. And apparently every time I thought I "just had a sinus headache", that was a migraine too. Borrowing Mandy's rescue medication sparingly here.
- Sometimes it's hard to sleep because it feels like the bed is shaking or that I am vibrating internally. It's hard to describe but that's the best that I can express it.
- And I am generally tired. I guess it takes a lot of enery for my brain to do things it's not supposed to be doing all the time.
What am I doing about it?
I'm working on figuring out my triggers for both the vestibuar migraines and PPPD. I definitely know (and have known for a long time) that aspartame (and any other artificial sweetener) gives me a migraine, which is disparaging since I wanted to cut out some sugar in my diet. I am limiting myself on sugary drinks and caffeine each day though. I was given a list of common migraine triggering foods and I cannot believe how much is on there. I know I don't need to cut them all out of my life - I just need to see which are problematic.
I'm now seeing a neurologist at Ohio State and we're trying medication out. I'm hoping for the best and will see how this plays out. He (and my ENT) did say if I don't feel the physical therapy is working to stop going. I do think I need to have some sort of vestibular rehabilitation but I will research some more and find something that will work for me. I think habituation and getting myself out doing things will help (without overdoing it and making me miserable). Plus hoping another major migraine attack doesn't just reset my progress.
I was worried that this will limit me with band camp (for my son's marching band) this summer and the upcoming marching season. However I'm not going to back down on volunteering and will do what I can as I've always have. I know I felt bad about not being able to be in the concession stand for this past basketball season but the tight quarters would not have done me any good.
I've joined a few subreddits regarding dizziness, vestibular migraines, and PPPD and I am going to start interacting with others with the same issues I'm facing.
I think I can get the vestibular migraine under control eventually and limit those episodes. I'm not sure if I'll ever get rid of the PPPD, from what I've read so far. I'm doing my due diligence and researching/reading more about it for a better understanding though.
Extra Resources
PPPD @ BalanceandDizziness.org
